Overview
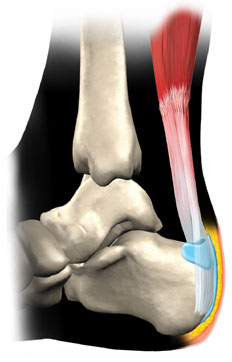 Achilles tendinitis is a common condition that causes pain on the back of the leg near the heel. The achilles tendon is the largest tendon in the body connecting your calf muscles to your heel bone. Your achilles tendon is used when you walk, run or jump. It is made to withstand a high amount of stress from these activities, but when it is overused, you can develop tendinitis. Tendinitis is defined as inflammation of a tendon. When you are injured, your body’s natural response causes inflammation. You may experience pain, swelling, or tenderness at the injured site. There are two types of achilles tendinitis, insertional and non-insertional achilles tendinitis.
Achilles tendinitis is a common condition that causes pain on the back of the leg near the heel. The achilles tendon is the largest tendon in the body connecting your calf muscles to your heel bone. Your achilles tendon is used when you walk, run or jump. It is made to withstand a high amount of stress from these activities, but when it is overused, you can develop tendinitis. Tendinitis is defined as inflammation of a tendon. When you are injured, your body’s natural response causes inflammation. You may experience pain, swelling, or tenderness at the injured site. There are two types of achilles tendinitis, insertional and non-insertional achilles tendinitis.
Causes
Achilles tendonitis is an overuse injury. Too much too soon is the common cause of overuse injuries, however other factors can contribute to developing the condition. An increase in activity, either distance, speed or a sudden change to running up hills. As a rule of thumb distance runners should increase their mileage by no more than 10% per week. A change of footwear or training surface for example suddenly running on soft sand can cause the heel to drop lower than normal making the tendon stretch further than it is used to. Weak calf muscles can tighten or go into partial spasm which again increases the strain on the achilles tendon by shortening the muscle. Running up hills – the achilles tendon has to stretch more than normal on every stride. This is fine for a while but will mean the tendon will fatigue sooner than normal. Overpronation or feet which roll in when running can place an increased strain on the achilles tendon. As the foot rolls in (flattens) the lower leg also rotates inwards which places twisting stresses on the tendon. Wearing high heels constantly shortens the tendon and calf muscles. When exercising in flat running shoes, the tendon is stretched beyond its normal range which places an abnormal strain on the tendon.
Symptoms
Morning pain is a hallmark symptom because the achilles tendon must tolerate full range of movement including stretch immediately on rising in the morning. Symptoms are typically localized to the tendon and immediate surrounding area. Swelling and pain at the attachment are less common. The tendon can appear to have subtle changes in outline, becoming thicker in the A-P and M-L planes. With people who have a tendinopathy of the achilles tendon that has a sensitive zone, combined with intratendinous swelling, that moves along with the tendon and of which sensitivity increases or decreases when the tendon is put under pressure, there will be a high predictive value that in this situation there is a case of tendinosis.
Diagnosis
Your physiotherapist or sports doctor can usually confirm the diagnosis of Achilles tendonitis in the clinic. They will base their diagnosis on your history, symptom behaviour and clinical tests. Achilles tendons will often have a painful and prominent lump within the tendon. Further investigations include US scan or MRI. X-rays are of little use in the diagnosis.
Nonsurgical Treatment
Achilles tendonitis will often respond to rest or changes in activity, stretching, or ice after activity. Non-steroidal anti- inflammatory drugs (NSAIDs), such as ibuprofen or naproxen may also help. Physical therapy focusing on stretching and strengthening, massage, alternating hot and cold baths, and ultrasound or sound waves can also help with healing and comfort. The temporary use of a heel lift or the insertion of an arch support, called an orthotic, into the shoe or sneaker can also help. Although seldom necessary, the ankle may be kept in a short leg cast or splint. Surgery is rarely needed but can remove bone spurs or the bony prominence of the heel bone. The injection of corticosteroids such as cortisone into the area of the Achilles tendon is usually avoided because it may cause the tendon to rupture.

Surgical Treatment
Mini-Open Achilles Tendon Repair. During a mini-open Achilles tendon repair surgery, 2 to 8 small stab incisions are made to pull the edges of the tendon tear together and suture the torn edges to repair the damage. During this procedure the surgeon will make one 3 to 4 cm long incision on the back of your ankle and 2 to 4 smaller vertical incisions around the long incision. These smaller veritical incisions are made with a pair of surgical scissors and are commonly referred to as “stab incisions”. Once the incisions are opened up, the surgeon will place precise sutures with non-absorbable stitches to strengthen the damaged Achilles tendon tissue. This suturing technique reduces the amount of scar tissue on the tendon after surgery and provides better surface healing of the skin. Unlike the traditional method of an open surgery, this procedure has less risks and complications involved. To learn about all risks you may face be sure to speak to your doctor.
Prevention
By properly training the body, an athlete can build the strength of their tendons and muscles. Following a workout and dieting plan, the body will be able to build muscle and strengthen most effectively. Additionally, doing the following can prevent tendinitis. Wearing appropriate shoes will give your foot the support it needs for proper movements of the foot and ankle. Improper movements will put additional stress on your body. Stretching before an athletic activity, Stretching primes the body for a taxing activity. Additionally, this will get your blood flowing and reduce the risk of pulling a muscle. Ask your doctor about orthotics, Custom orthotics can help get your foot into proper alignment. If the foot does not execute proper mechanics, the body will adjust which will cause pain and increase the chances of injury.
 Achilles tendinitis describes an inflammatory change of the Achilles tendon without a tear of the tendon. Achilles tendinitis may be acute or chronic. The onset of pain is usually unilateral but may be found bilaterally. Achilles tendinitis is common in the third or fourth decade of life in patients who are active with sports or in jobs that require physical labor. Pain is described at the insertion of the tendon in the heel bone or in the body of the tendon.
Achilles tendinitis describes an inflammatory change of the Achilles tendon without a tear of the tendon. Achilles tendinitis may be acute or chronic. The onset of pain is usually unilateral but may be found bilaterally. Achilles tendinitis is common in the third or fourth decade of life in patients who are active with sports or in jobs that require physical labor. Pain is described at the insertion of the tendon in the heel bone or in the body of the tendon.